- Регистрация
- 17 Фев 2018
- Сообщения
- 42,480
- Реакции
- 0
- Баллы
- 36
Ofline
Doctors suspect three factors, each unremarkable on its own, contributed to his fate.
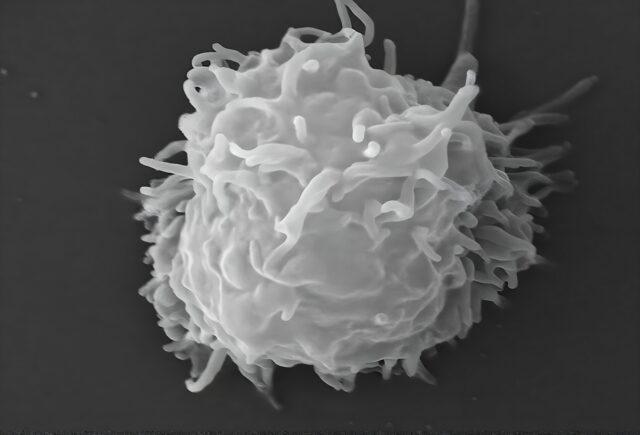
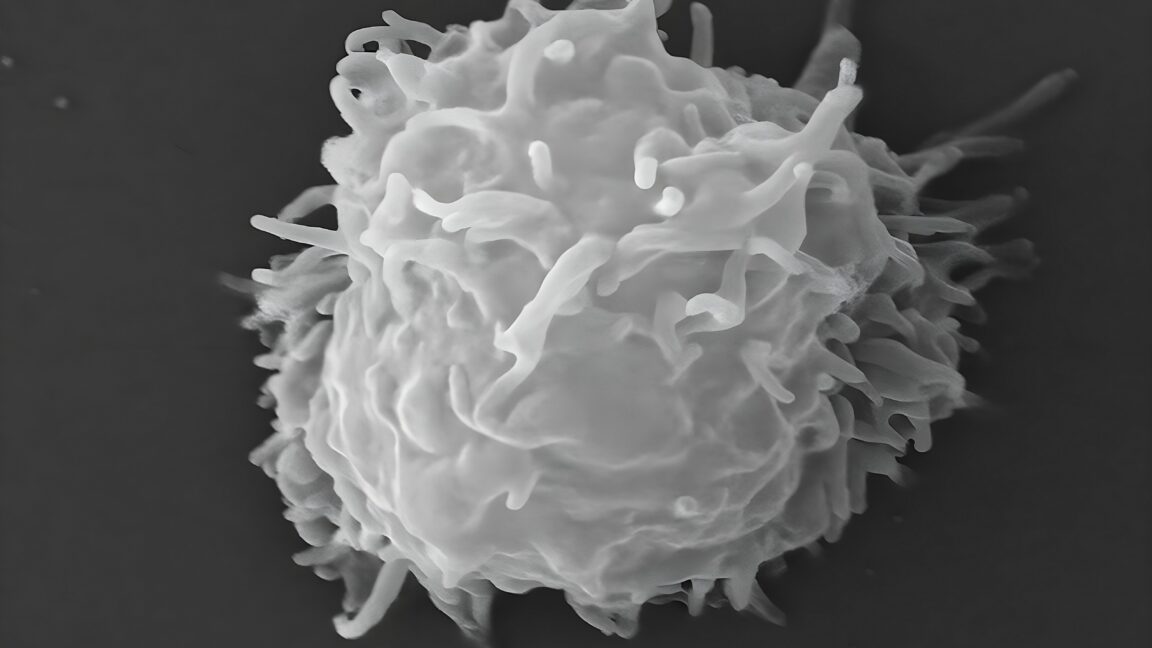
This scanning electron microscope (SEM) image revealed some of the ultrastructural features observed on the surface of a protozoan Acanthamoeba polyphaga. Credit: Getty | CDC
Over the course of six months, black lesions and deep ulcers formed over the body of a 78-year-old man, puzzling doctors. His face was covered in dark scabs. A lesion had destroyed his left eyelid, and one had created a hole between the roof of his mouth and his nasal cavity.
It wasn’t until he was transferred to a Yale School of Medicine hospital for higher-level care that doctors finally identified the cause of his ghastly affliction: a common free-living amoeba that can be found almost anywhere, including tap water. But by then, it was too late. The man’s case is reported in the journal Emerging Infectious Diseases. (A graphic image of his case is here, but be warned.)
The amoeba the doctors found was Acanthamoeba, which is known to cause such horrifying infections. But it’s rare, and when it explodes into a full-body, often deadly malady, it tends to be in patients who have compromised immune systems or are otherwise debilitated. As such, the opportunistic pathogen is most often found in people with HIV/AIDS, cancers, and diabetes, as well as those on powerful immunosuppressive drugs, like transplant patients. The man didn’t fit into any of these categories.
Besides widespread infections, Acanthamoeba is known to cause localized ones, most notably eye infections—aka Acanthamoeba keratitis. It’s rare, but often linked to contact wearers who don’t clean their lenses properly. If not identified and treated early, it can easily lead to permanent vision loss. The unicellular terror can also cause a rare brain infection (granulomatous amebic encephalitis), again, mostly in immunocompromised patients. And it can infect wounds or the sinuses, particularly in people who rinse their sinuses with tap water that hasn’t been boiled. Acanthamoeba and other amoeba species have been found in more than 50 percent of US tap water samples.
Of all the known ways to get an Acanthamoeba infection, nasal rinsing was the most likely one in the man’s case. The man had nasal polyps and used sinus rinses to alleviate his symptoms. However, his symptoms didn’t start in his nasal passages—they started on his legs. There, red nodules formed and progressed to develop dark centers. Some became deep ulcers, while others became necrotic, turning to black scabs. Then began erupting on his trunk, arms, and neck.
Before his transfer to Yale, doctors elsewhere tried to identify the mysterious cause, doing multiple biopsies of his diseased skin. Tests were negative for bacterial or fungal pathogens. But they showed his blood vessels were inflamed and full of clumps of immune cells. Doctors worried that his immune system was attacking his blood vessels, causing the necrotic lesions. So, they put him on immunosuppressant drugs. But his condition only worsened, and the lesions only progressed. When he arrived at Yale, he had a fever and high heart rate, and appeared frail. He had lost 16 pounds and was drowsy and confused. He was blanketed in lesions.
The Yale doctors noted that the lesions began after he returned from Florida, where he spent the winters. While there, he was exposed to a red tide (caused by algae) while cleaning up after a hurricane. Otherwise, he had a medical history of just the nasal polyps and asthma, which he treated with a monoclonal antibody drug, dupilumab. Given that his lesions progressed, they redid a skin biopsy, this time finding cells that looked like amoebas. DNA testing confirmed Acanthamoeba.
The doctors quickly put him on a five-drug regimen recommended for such infections by the Centers for Disease Control and Prevention, but he continued to deteriorate. They then sought and got approval from the Food and Drug Administration for a single-patient experimental trial of an antibiotic (nitroxoline) that had shown success in treating a different amoeba in another patient. Once the doctors started it in the man, it appeared to work. His fever broke briefly, some of his lesions improved, and no new ones formed.
But the improvements were short-lived. His kidney function worsened, and doctors took him off the drugs to prevent further damage. His lesions showed signs of secondary infections and multiorgan failure developed. He died six weeks after the amoeba infection was identified.
The doctors were left to speculate on how he met such a gruesome end. The nasal rinses were the most obvious route of exposure. His old age and declining immune responses may have played a role, too, they speculate. But they also looked at the one medication he was on: dupilumab.
It’s a monoclonal antibody that inhibits certain immune signals, namely interleukin-4 and interleukin-13 cytokines, which play a role in overactive (T2) inflammatory responses. The doctors noted that other drugs targeting T2 inflammatory responses have been linked—in rare cases—to parasitic infections. A trial of dupilumab that included over 400 children reported that six children given the drug developed parasitic worm infections, while there were no such cases in the control group. The researchers leading the trial concluded at the time that the worm infections weren’t related to dupilumab. But the Yale doctors wondered if maybe they had been.
“Although dupilumab is not classically considered an immunosuppressive agent, it possibly increases the risk for parasitic infections,” they wrote.
Overall, they speculate that the drug may have been one factor among several—including nasal rinsing and age—that led to the man’s amoeba infection. While further data will be needed to firm up any link, the researchers highlight that physicians shouldn’t overlook potential signs of free-living amoebas.


This scanning electron microscope (SEM) image revealed some of the ultrastructural features observed on the surface of a protozoan Acanthamoeba polyphaga. Credit: Getty | CDC
Over the course of six months, black lesions and deep ulcers formed over the body of a 78-year-old man, puzzling doctors. His face was covered in dark scabs. A lesion had destroyed his left eyelid, and one had created a hole between the roof of his mouth and his nasal cavity.
It wasn’t until he was transferred to a Yale School of Medicine hospital for higher-level care that doctors finally identified the cause of his ghastly affliction: a common free-living amoeba that can be found almost anywhere, including tap water. But by then, it was too late. The man’s case is reported in the journal Emerging Infectious Diseases. (A graphic image of his case is here, but be warned.)
Unicellular terror
The amoeba the doctors found was Acanthamoeba, which is known to cause such horrifying infections. But it’s rare, and when it explodes into a full-body, often deadly malady, it tends to be in patients who have compromised immune systems or are otherwise debilitated. As such, the opportunistic pathogen is most often found in people with HIV/AIDS, cancers, and diabetes, as well as those on powerful immunosuppressive drugs, like transplant patients. The man didn’t fit into any of these categories.
Besides widespread infections, Acanthamoeba is known to cause localized ones, most notably eye infections—aka Acanthamoeba keratitis. It’s rare, but often linked to contact wearers who don’t clean their lenses properly. If not identified and treated early, it can easily lead to permanent vision loss. The unicellular terror can also cause a rare brain infection (granulomatous amebic encephalitis), again, mostly in immunocompromised patients. And it can infect wounds or the sinuses, particularly in people who rinse their sinuses with tap water that hasn’t been boiled. Acanthamoeba and other amoeba species have been found in more than 50 percent of US tap water samples.
Of all the known ways to get an Acanthamoeba infection, nasal rinsing was the most likely one in the man’s case. The man had nasal polyps and used sinus rinses to alleviate his symptoms. However, his symptoms didn’t start in his nasal passages—they started on his legs. There, red nodules formed and progressed to develop dark centers. Some became deep ulcers, while others became necrotic, turning to black scabs. Then began erupting on his trunk, arms, and neck.
Catching a killer
Before his transfer to Yale, doctors elsewhere tried to identify the mysterious cause, doing multiple biopsies of his diseased skin. Tests were negative for bacterial or fungal pathogens. But they showed his blood vessels were inflamed and full of clumps of immune cells. Doctors worried that his immune system was attacking his blood vessels, causing the necrotic lesions. So, they put him on immunosuppressant drugs. But his condition only worsened, and the lesions only progressed. When he arrived at Yale, he had a fever and high heart rate, and appeared frail. He had lost 16 pounds and was drowsy and confused. He was blanketed in lesions.
The Yale doctors noted that the lesions began after he returned from Florida, where he spent the winters. While there, he was exposed to a red tide (caused by algae) while cleaning up after a hurricane. Otherwise, he had a medical history of just the nasal polyps and asthma, which he treated with a monoclonal antibody drug, dupilumab. Given that his lesions progressed, they redid a skin biopsy, this time finding cells that looked like amoebas. DNA testing confirmed Acanthamoeba.
The doctors quickly put him on a five-drug regimen recommended for such infections by the Centers for Disease Control and Prevention, but he continued to deteriorate. They then sought and got approval from the Food and Drug Administration for a single-patient experimental trial of an antibiotic (nitroxoline) that had shown success in treating a different amoeba in another patient. Once the doctors started it in the man, it appeared to work. His fever broke briefly, some of his lesions improved, and no new ones formed.
But the improvements were short-lived. His kidney function worsened, and doctors took him off the drugs to prevent further damage. His lesions showed signs of secondary infections and multiorgan failure developed. He died six weeks after the amoeba infection was identified.
Speculation on multifactor infection
The doctors were left to speculate on how he met such a gruesome end. The nasal rinses were the most obvious route of exposure. His old age and declining immune responses may have played a role, too, they speculate. But they also looked at the one medication he was on: dupilumab.
It’s a monoclonal antibody that inhibits certain immune signals, namely interleukin-4 and interleukin-13 cytokines, which play a role in overactive (T2) inflammatory responses. The doctors noted that other drugs targeting T2 inflammatory responses have been linked—in rare cases—to parasitic infections. A trial of dupilumab that included over 400 children reported that six children given the drug developed parasitic worm infections, while there were no such cases in the control group. The researchers leading the trial concluded at the time that the worm infections weren’t related to dupilumab. But the Yale doctors wondered if maybe they had been.
“Although dupilumab is not classically considered an immunosuppressive agent, it possibly increases the risk for parasitic infections,” they wrote.
Overall, they speculate that the drug may have been one factor among several—including nasal rinsing and age—that led to the man’s amoeba infection. While further data will be needed to firm up any link, the researchers highlight that physicians shouldn’t overlook potential signs of free-living amoebas.
